- To have a timely and peaceful transition?
- To get complete relief from unbearable pain and suffering?
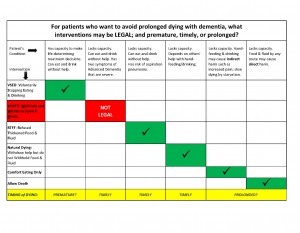
- To avoid prolonged harm and burdens if you reach Advanced Dementia?
- To have others honor your dignity and respect your privacy?
- To protect your family members from stress and conflict?